Modern Spacious Clinic
Foot Health Clinic, located at Samford Village in Brisbane's northside, is a Brisbane kids, family and active adventurers podiatry clinic.
We are recognised Foot and Ankle Professionals. Our podiatry clinic has been established in Brisbane's northside for over 20 years and during this time we have helped thousands of people.
We offer a complete range of podiatry services for kids, families and active adventurers and we offer a range of footwear related products.
We typically treat podiatry patients from the surrounding Brisbane suburbs of Albany Creek, The Gap, Bridgeman Downs, Ferny Hills, Mitchelton, Arana Hills, Eatons Hill, Ferny Hills, Keperra, McDowall and Upper Kedron.
We are proud sponsors of the Samford Rangers Football Club, the Samford Show and the Samford Fun Run.

Our specialities
Kids
Families
Active Adventurers
Why Foot Health Clinic?
Timely support
At Foot Health Clinic we aim to arrange an appointment which suits you and at your earliest convenience. We can accommodate most appointments within 1 week.
Innovative Ideas
Our Clinic introduced Ingrown toenail bracing to Australia – a revolutionary non-surgical treatment. By continuing Professional development we stay up to date with developments and advances in foot care.
Advanced Technology
Foot Health Clinic is at the forefront of new technology and our clinic offers an onsite CAD/CAM Orthotic laboratory. In addition, we have advanced treatment technology including Thor Laser and Lunula Fungal Nail Laser.
Clear Communication
Our Clinic has invested significant time and energy into developing a stream-lined assessment and diagnosis process. We discuss our findings with you and give you a clear indication of your treatment options
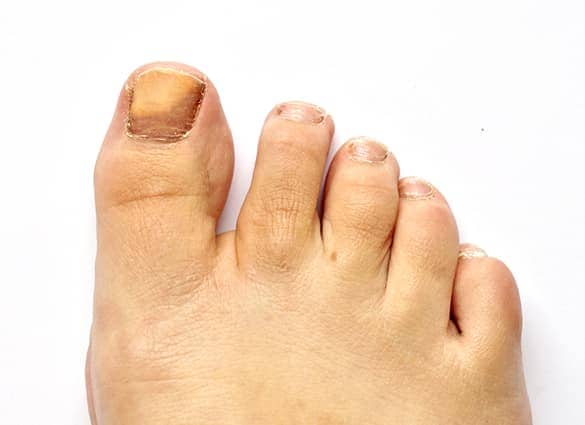
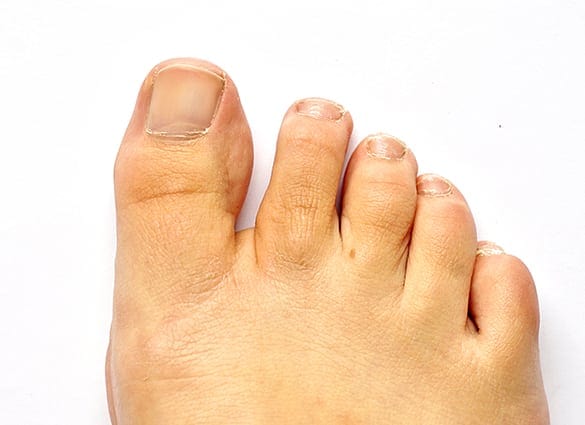
Fungal Laser Treatment
Until recently, fungal toenail infections were treated with antifungal nail lacquers or oral medication.
Antifungal toenail lacquers have not proven to be very effective and patients have experienced poor success rates. With oral medications there is the risk of side effects such as liver toxicity and this is generally not a preferred option.
Fortunately, medical technology has introduced a revolutionary method of treating fungal nail infection that’s not only effective, but is 100% safe and has no side effects.
Find your pain
Each of our Podiatry services is designed to get to the root of your foot problem so we treat the underlying cause rather than just addressing symptoms. We encourage you to make an appointment with our podiatrists to discuss your pain. If you’d like to learn more about possible causes of your pain before your appointment, please point to the area of the foot or ankle where it hurts and click the target to discover more. This is not to be used as a substitute for medical advice and it is not intended to be used to diagnose, treat, cure or prevent any disease or therapeutic purposes.
Areas We Service For Podiatry.
Looking for a podiatry clinic in Samford Village or near the surrounding suburbs? Our clinic is conveniently located Samford Central Shopping Centre, Cnr Mt Glorious Rd & Mary Ring Dr, Samford Village QLD 4520.
To easily find us: Get Directions From Your Location.
Foot Health Clinic offers podiatry services for residents throughout Brisbane North, including Albany Creek, Arana Hills, Bridgeman Downs, Eatons Hill, Ferny Hills, Keperra, McDowall, Mitchelton, The Gap and Upper Kedron.